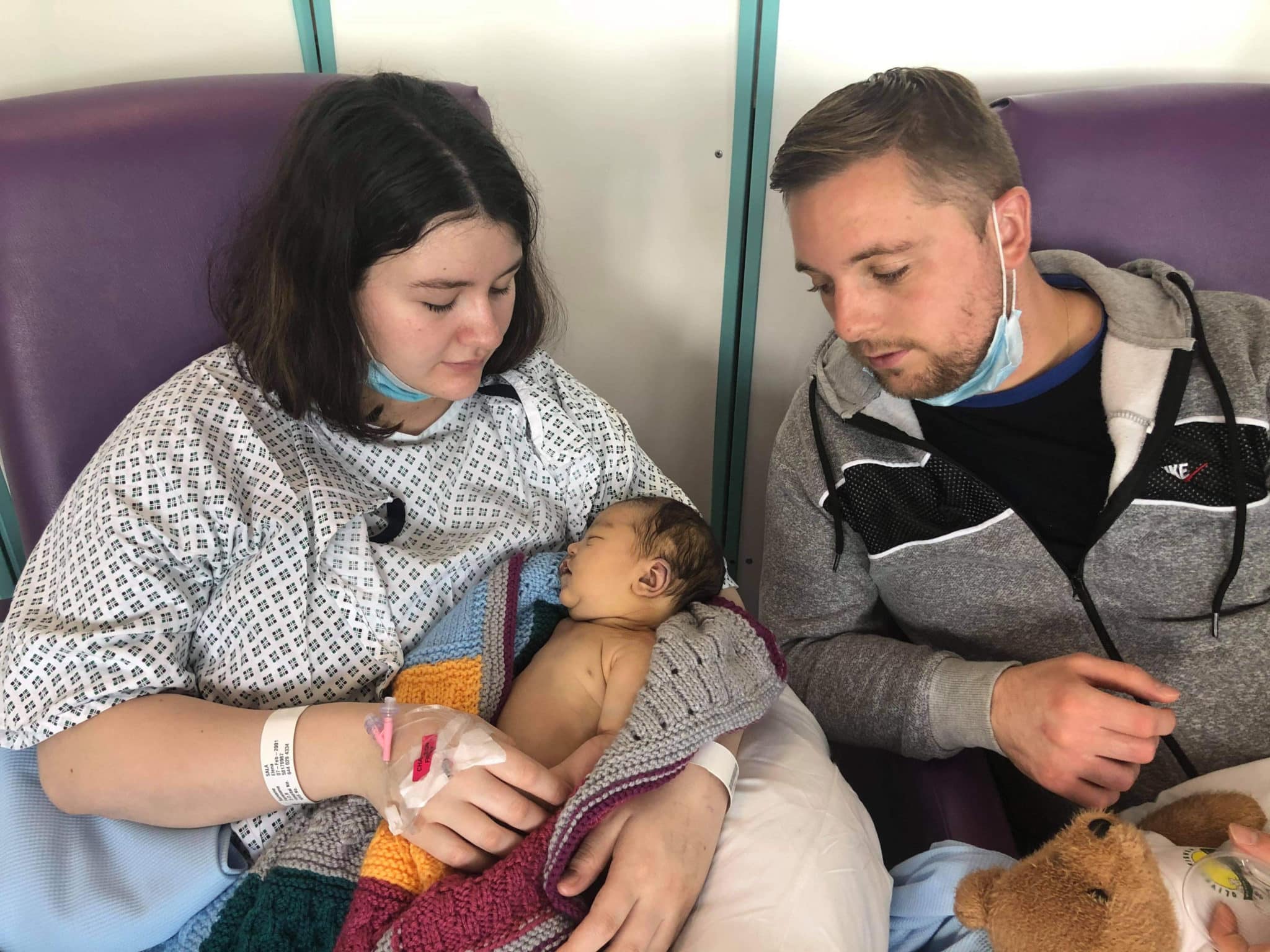
Parents of a baby who died at Tunbridge Wells Hospital nearly two years ago have been told they will have to wait until the end of the month to discover a coroner’s findings into the death.
Rosanna Matthews was delivered on November 20, 2020, at Tunbridge Wells Hospital. She was born without a heartbeat and after resuscitation was placed into a coma for three days but later died.
Her mother, Elena Sala, believes if she had been allowed to start pushing at 3pm when she first started to feel the urge, rather than waiting until 4.45pm under the advice of midwives, Rosanna would have lived.
After nearly two years of delays, an inquest into Rosanna’s death was conducted at the Archbishop’s Palace in Maidstone last week, but the coroner’s conclusion will not be delivered until the end of the month.
Coroner Catrina Hepburn said the reason for the delay could not be stated in open court and addressed the family directly, saying: “I’m sure you’re disappointed but I’m sure you would rather we cover everything as thoroughly as possible.”
In court, Ms Sala claimed midwives were ‘bickering’ and appeared confused during her labour, while midwives claimed she had declined an internal examination twice – though Ms Sala says she only declined once.
The head of midwifery at Maidstone and Tunbridge Wells NHS Trust (MTW), which runs the hospital, admitted there were ‘errors in communication’ between midwives and the mother.
Rachel Thomas, who was deputy head of gynaecology and midwifery at the time of Rosanna’s birth, said MTW had taken steps to reduce similar events reoccurring.
“We actually now review complaints we’ve received and concerns raised about their experiences, and we’ve produced an infographic we give to women to explain some of the reasons why we might do the examination,” she explained.
“It’s extremely important for us to take on board any learning identified in internal and external reports.
“We have had foetal surveillance consultants in place since December 2021 and foetal surveillance midwives in place since May 2020, to look at foetal heart rate monitoring, and we have increased consultant presence on the labour ward to seven days a week from 7am until 9pm.
“We have updated our guidance so it’s easier to follow, with flow charts in place.
“We’ve introduced a masterclass for all our doctors and staff that’s very clear about what issues need to be present to do an instrumental delivery.”
She added that every single one of the approximately 6,000 births per year within the trust will now be audited